The WebApp is sponsored by: 

Reasons for deferral and denial in living donor candidates: a single-center exploratory study
Kathryn Czepiel1, Lourdes Chua2, Brandon Bassett3, Sarah Samreth3, Annette Nasr4, Faith Borunda3, Noelle Ebel1, Leina Alrabadi1, Amrita Narang1, Roger Sands5, Varvara Kirchner6.
1Department of Pediatrics, Division of Gastroenterology, Hepatology and Nutrition, Stanford University, Palo Alto, CA, United States; 2Stanford Health Care, Palo Alto, CA, United States; 3Stanford Medicine Children's Health, Palo Alto, CA, United States; 4Department of Pediatrics, Stanford University, Palo Alto, CA, United States; 5Department of Medicine, Division of Gastroenterology and Hepatology, Stanford University, Palo Alto, CA, United States; 6Department of Surgery, Division of Abdominal Transplantation, Stanford University, Palo Alto, CA, United States
Introduction: Identification of and access to a potential living donor for children awaiting liver transplantation is associated with a survival benefit. Despite a high volume of living donor applications at our transplant center, few living-donor transplant operations are performed annually for pediatric recipients. We sought to improve transparency and gain an understanding of reasons why a living donor candidate may be deferred or denied for living donor transplantation.
Method: We developed a multi-disciplinary quality improvement team comprised of a living donor nurse coordinator, living donor advocate, transplant surgeon, pediatric and internal medicine-trained transplant hepatologists, an improvement science expert, data analyst, and transplant center leadership to evaluate the donor candidate application process. Using survey methodology, we prospectively collected information on factors motivating organ donation and the intermediary outcomes for candidates as they progress from candidacy screening to in-person medical evaluation to transplant operation.
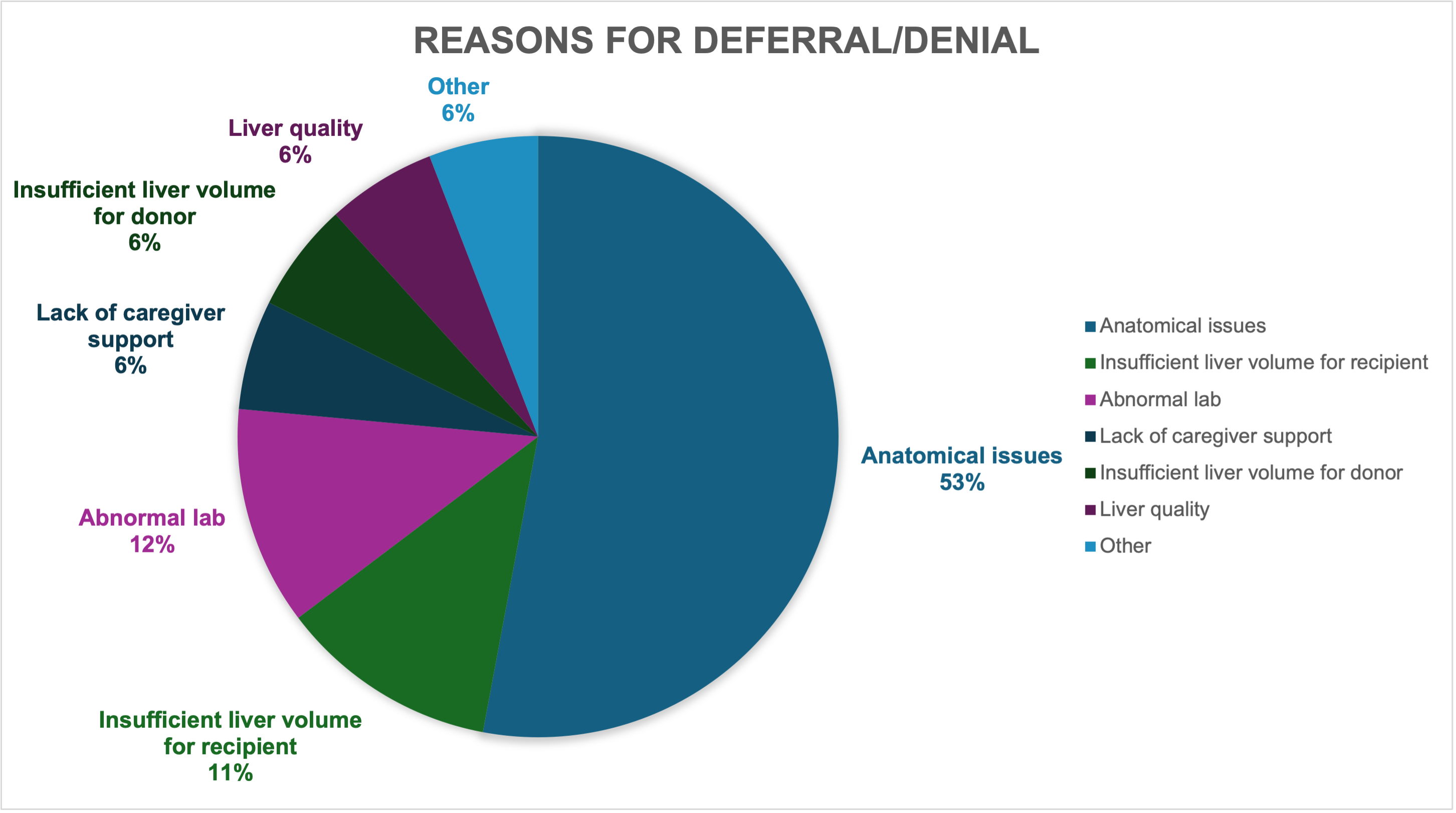
Results: Of 29 living donor applicants who completed medical evaluation, 13 were accepted (44.8%), 1 was deferred (3.4%), and 15 were denied (51.7%). An anatomical issue was the most cited reason for deferral/denial (N=9, 56.3%). Other commonly cited reasons for deferral/denial include insufficient liver volume for recipient (N=2), recipient received cadaveric donation (N=2), abnormal labs (N=2), insufficient liver volume for donor (N=1), liver quality (N=1), and lack of caregiver support (N=1) (Figure 1). Donor medical issues, financial limitations, psychosocial issues, and concern for donor coercion were not cited as reasons for deferral/denial.
Conclusion: Over half of our living donor applicants are deferred or denied due to anatomical issues.
This work was supported by grants from The Lillie and Donnelly Seed Grant Program through the Stanford Medicine Center for Improvement and The Association of Auxiliaries for Children through the Lucile Packard Foundation..
Email: info@splitmeeting.org
If you have any questions during the meeting, please go to the registration desk. Our emails will be monitored sporadically.
REGISTRATION DESK OPENING TIMES